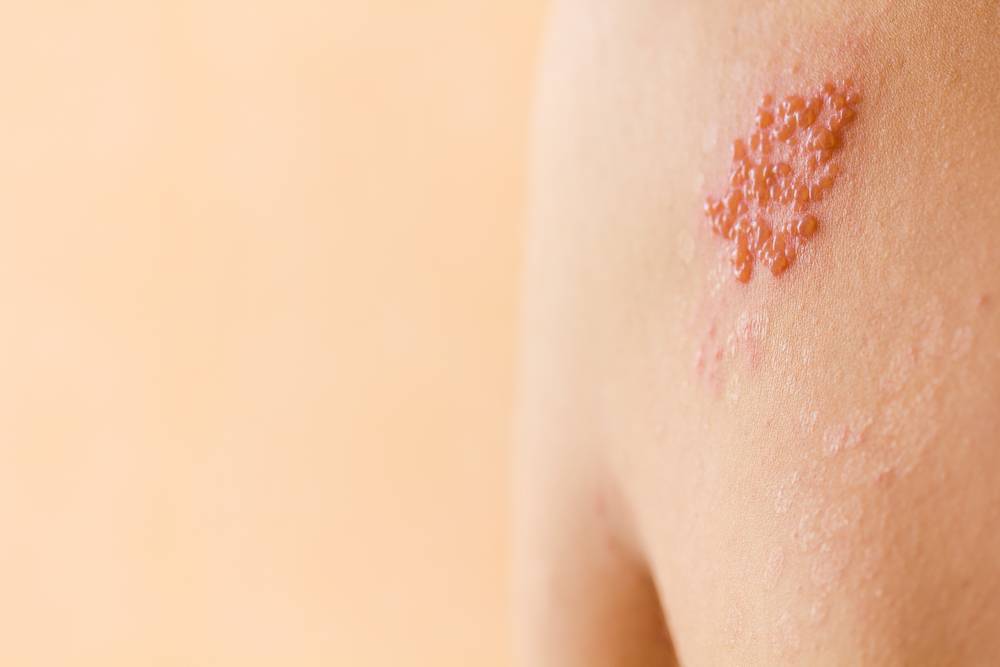
Shingles, also known as herpes zoster, is a painful rash caused by varicella zoster virus (VZV), the same virus responsible for Chickenpox. After recovery from Chickenpox, VZV stays dormant in the nerves. The virus can reactivate later in life, multiplying along the nerves to the skin, manifesting as an excruciating band of blisters – a hallmark of Shingles.
Causes and Transmission
As mentioned above, shingles is caused by the reactivation of the Chickenpox VZV – You cannot get Shingles if you have never had Chickenpox.
In a nutshell, how a person gets Shingles:


What causes the reactivation of VZV?
VZV reactivates to cause Shingles when the immune system is weakened, as in the following groups:
- Being >50 years old: the risk of Shingles increases with age as immunity naturally declines with age.
- Having certain diseases e.g. HIV/AIDS and cancer that can compromise the immune system
- Prolonged use of certain medications which lower immunity e.g. immunosuppressants, steroids, chemotherapy
- Being under a lot of stress
How is VZV spread?
People with shingles cannot spread VZV before their rash blisters appear, or after the blisters scab. They are contagious only during the blister stage; touching the fluid from the blisters will spread VZV.
People with chickenpox are more likely to spread VZV than people with shingles. They are contagious 1-2 days even before rash appears, until blisters scab. Furthermore, VZV in chickenpox can be spread in the air through coughing or sneezing.
Complications
Some of the possible complications of Shingles even after the rash clears include:
- Postherpetic Neuralgia (PHN) or long-term nerve pain
- Those >40 years of age are more predisposed to developing PHN.
- Affects ~10-18% of people who have had Shingles, occurring where the rash was and persisting for months or years.
- Pain may be debilitating and necessitate treatment.
- Vision loss if it occurs in or near the eye
- Neurological problems e.g. facial paralysis, brain inflammation (encephalitis)
- Bacterial infection of skin lesions
- Hearing and balance problems, if Shingles appears in or around the ear
Signs and Symptoms
Several days before the characteristic shingles rash appears, people may experience pain, itching, or tingling in the area where the rash will develop.
The rash usually occurs as a single stripe of blisters on one side of the face or body. The blisters scab over in 7 to 10 days, usually clearing up within 2 to 4 weeks.
Rarely, Shingles presents without rash. In such cases it is termed Zoster Sine Herpete (ZSH).
Other non-specific signs and symptoms include fever, headache, fatigue, chills, nausea.
Diagnosis
The signs and symptoms are usually distinctive enough to accurately diagnosis Shingles. In the rare instances of ZSH, Polymerase Chain Reaction (PCR) testing may be done to detect VZV DNA in swabs of lesions.
Treatment
There is no cure for Shingles, and treatment usually involves:
- Symptomatic relief
- Antihistamines for itch
- Anti-inflammatory drugs e.g. ibuprofen for pain and swelling
- Antivirals (e.g. Acyclovir, Famciclovir, Valacyclovir) to shorten the duration of the illness, and reduce risk of complications.
- Anticonvulsants e.g. Gabapentin or tricyclic antidepressants e.g. Amitryptyline that help with neuropathic pain in complicated cases
Prevention
- Avoid direct contact with the blisters of an infected person
- Avoid touching items that may have touched their rash e.g. clothes, towels, bedding.
- Wash hands frequently if exposure is unavoidable.
- To prevent stress-induced reactivation: try to get sufficient sleep, eat a healthy, well-balanced diet and exercise regularly or engage in activities to relax your mind.
- Vaccinations are available that can:
- Protect people from VZV
- Even after they have already had Chickenpox e.g. Shingrix
Shingrix
- FDA-approved for the prevention of shingles in adults ≥50 years of age
- A nonliving vaccine made of a virus component, given in 2 doses, 2-6 months apart
- Shown to offer ~90% protection for ~5 years in clinical trials
Vaccinations are not a guarantee against shingles but will reduce duration and severity of illness, also minimising complications.