
Rat Infestation In Singapore: Why Is It Worrying?
Rats can carry and spread infectious diseases. When they roam about, their feces, urine, or

Rats can carry and spread infectious diseases. When they roam about, their feces, urine, or

The respiratory illness bronchiectasis should not prevent you from living your best life. Simple lifestyle

Surviving an earthquake can be a traumatic and life-changing event, and the aftermath can have
Pfizer’s PENBRAYA vaccine transforms meningitis protection with comprehensive coverage and fewer shots. Read more
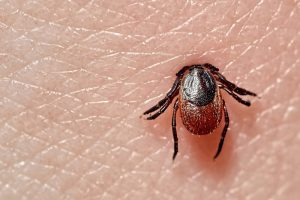
The prevalence of Lyme disease in Asia, a region where this tick-borne illness was previously less common, is now being increasingly recognised. A systematic review

In a world where technological advancements continuously reshape various aspects of life, healthcare is no exception. The National University Hospital (NUH) in Singapore has made a significant leap in this direction by implementing an Artificial Intelligence (AI) triage tool called RapidAI. This AI tool, capable of identifying stroke patients in less than a minute, is revolutionising the way healthcare providers approach stroke management. By significantly reducing the diagnosis time, it enables faster treatment decisions, thereby improving patient outcomes and potentially transforming stroke care in Singapore and beyond.




