
Medical Channel Asia Launches Community Forum Connecting Readers with Doctors
Medical Channel Asia has launched an innovative community forum to bridge the gap between readers

Medical Channel Asia has launched an innovative community forum to bridge the gap between readers

In recent years, a popular solution for hairloss has been CosmeRNA, a product which has
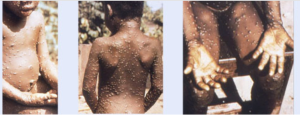
The World Health Organization (WHO) declared on 11 May 2023 that the mpox outbreak is
Hallux limitus is a common foot condition that affects a significant number of people, particularly in Asia. It is a form of arthritis that affects the joint at the base of the big toe, known as the first metatarsophalangeal joint (MTPJ).
The inflammation of joints is known as arthritis. It is not a single disease entity but a general term used for a wide variety of
It has been estimated that Asia will be the fastest growing region for genetic testing in the coming 5 years. Find out 5 facts about it here.




