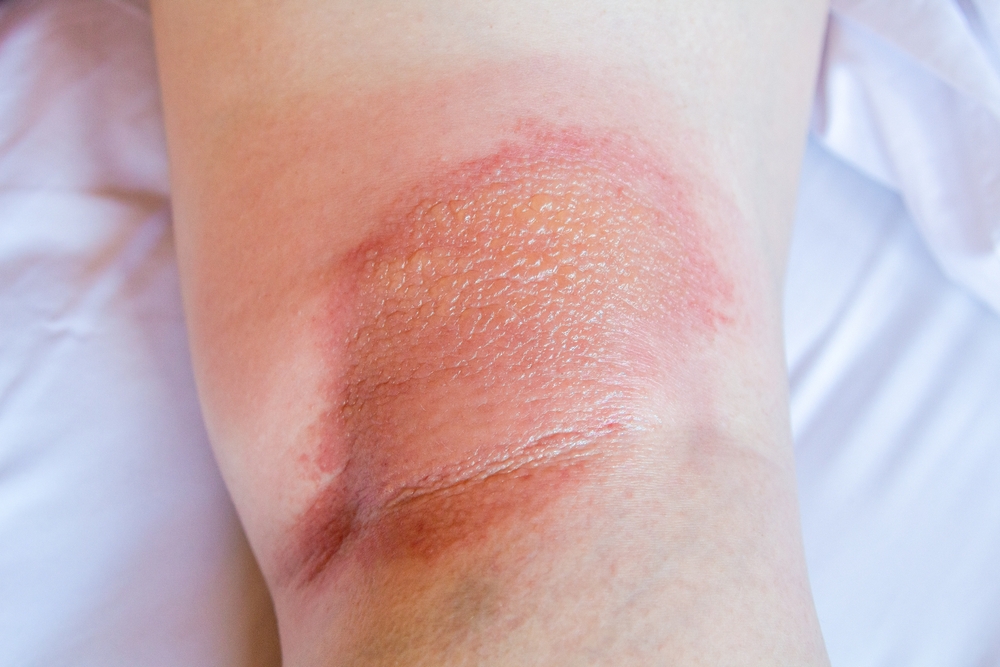
Atopic dermatitis, or commonly known as eczema, is a common chronic inflammatory skin condition characterised by itchy skin accompanied with a red rash. It occurs when patches of skin become itchy, red or cracked. Genetic factors and environmental conditions play a large role in contributing to the pathogenesis of eczema.
Epidemiology
Globally, 15 to 20 percent of children have atopic dermatitis. Children born to Asian parents have the highest eczema risk in the world, with nearly 30 percent of infants developing the condition in the first year. The onset of atopic dermatitis usually presents by five years of age, with the highest incidence between three and six months of age. Symptoms usually resolve by adulthood but around 10 – 20 percent of patients will have persisting symptoms.
Types of Eczema
- Contact Dermatitis occurs when there is contact with an irritant. This can cause itching, inflammation that results in redness and a burning sensation being felt. This type of eczema is temporary and will usually clear once the irritant has been removed or washed off, with symptoms clearing quickly after.
- Nummular Dermatitis usually occurs during the winter months or when the weather becomes extremely dry. This can cause dry patches of skin, especially on the legs.
- Dyshidrotic dermatitis is very common in women and causes itchy, scaly, painful patches of skin that can turn red.
Symptoms of Eczema
Atopic eczema signs and symptoms vary from person to person. Symptoms can subside and flare up depending on multiple factors including temperature, humidity levels and the amount of irritant causing inflammation. Eczema can usually be seen on the arms, face, chest, inner elbows, in between joints and the back of the knees.
Some common symptoms include:
- Intense itching which may be especially severe during the night
- Small, raised bumps which may leak fluid when scratched
- Cracked, scaly and thickened skin
- Raw and sensitive skin
- Red to brownish-grey patches
What causes eczema?
The most common cause is due to direct skin contact with something that causes inflammation in the skin (irritant). Eczema is a result of an overactive immune system that responds excessively when exposed to irritants or triggers.
Genetic predisposition is a strong factor in causing atopic dermatitis, but etiological details of inheritance are still poorly understood. Atopic dermatitis is associated with mutations in the FLG gene, responsible for important substituents of the superficial layer of the skin (epidermis).
Parents who have allergic disorders such as atopic dermatitis, allergic rhinitis, hay fever or asthma may also be prone to having children with atopic dermatitis. Around half of patients with severe atopic dermatitis will also develop asthma.
Atopic dermatitis can occur at any age, with the greatest risk in children. The condition usually improves in adulthood but can persist in more than half of those who suffer from it. The likelihood of developing atopic dermatitis increases with the number of risk factors or triggers one is sensitive to.
Common Eczema Triggers
Sweat
Excessive sweat that is not wiped off can trap moisture, especially between joints. This build-up of moisture can cause eczema because our sweat contains chemicals that cause imbalance to the skin’s natural barrier, leading to irritation.
Stress
Psychological stress can increase atopic dermatitis. Research has shown that eczema can be exacerbated by stress which induces a greater amount of skin inflammation. This is because stress can produce neuroendocrine mediators which activates local inflammation of the neurones innervating the skin and disrupting skin barrier function.
Dry Skin
Sensitive skin or the lack of moisturising, especially in countries with high content of chlorine in water, can lead to one being extra sensitive and susceptible to inflammation.
Abrasions
Tiny superficial skin abrasions invisible to the naked eye can result from prolonged wear of rough clothing, or having skin contact with certain furnishings. These tears allow for bacteria to grow which may also result in an infection.
Other factors
- Humidity
- Skin irritants such as drying chemical agents found in cosmetic products, detergents, perfumes, dust and chlorine.
- Other allergies that occur in tandem with eczema e.g. allergic rhinitis
- Upper respiratory infections
Eczema is not a skin infection but a type of skin irritation. Scratching causes further inflammation and may lead to abrasions which allow opportunistic infectious organisms to enter the skin.
Prevention
Moisturising
Applying a clinically and dermatologically certified moisturiser can help to alleviate dry skin by providing a superficial layer of moisture to help protect the skin from becoming easily injured from tiny abrasions. Creams and ointments are better than lotions which may contain skin irritants such as preservatives or lanolin.
Countering excessive hand washing
Constant scrubbing and frequent washing of the hands can gradually diminish the protective skin barrier and lead to the loss of the skin’s natural oils. Moreover, some soaps contain strong chemicals that can further irritate this thin barrier. To counter this, use mild fragrance-free soaps. Hands should also be pat dry before moisturising.
Avoid scratching
Scratching breaks the skin. It can help to rub gently, rather than scratch as skin infections such as impetigo can develop where there are openings in the skin for bacteria to enter.
Clinical Intervention
- Oral antihistamines such as fexofenadine (Allegra) and loratadine (Claritin) may help to relieve itching where they block histamine, a chemical released by the body that triggers inflammation and allergic reactions.
- Steroidal creams to relieve scaling
- Low-potency steroids e.g. hydrocortisone
- Phototherapy (light therapy) that uses ultraviolet light to reduce eczema
- Oral steroids such as prednisolone suppress the immune system. These are used temporarily to control severe eczema flares and not for long term usage.