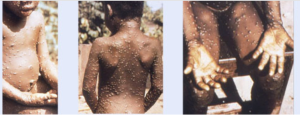
WHO Announced the End of Mpox as Global Health Emergency
The World Health Organization (WHO) declared on 11 May 2023 that the mpox outbreak is


The World Health Organization (WHO) declared on 11 May 2023 that the mpox outbreak is

Discover five lesser-known health conditions that impact men’s well-being in Asia, and learn how to

Testicular torsion happens most commonly between ages 12 and 18. Read this article to find
Endometriosis is a painful disorder of the uterine lining that affects approximately 10 to 15 percent of women worldwide during their reproductive age. While it
Fungal infection of the nail is termed onychomycosis. Different fungal organisms may infect the nails with different presentations affecting any part of the nail including
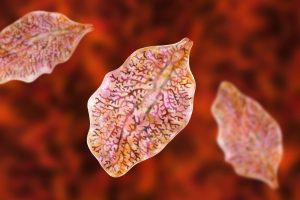
Liver flukes are parasitic flatworms wreak havoc on human health, particularly in areas with poor sanitation and widespread consumption of raw or undercooked fish.




