While fatty liver dominates headlines, many in Asia suffer from rare liver diseases that are often misdiagnosed; here is how modern medicine identifies these hidden conditions.
When people visit a liver clinic, they usually worry about alcohol, fried food, or viral hepatitis. These are indeed the big players in liver health across Asia. However, the liver is an incredibly complex organ, and sometimes, the issues we face are not about what we eat or drink, but about the unique genetic and biological blueprint we were born with.
Rare liver diseases often hide in plain sight. Because their symptoms—like fatigue or itchy skin—seem so ordinary, many patients go years without a correct diagnosis. In this article, we explore five rare liver diseases, their impact on the body, and why awareness is the first step towards prevention and management.
Alpha-1 Antitrypsin Deficiency: Protein Misfolding
Most people think of the liver as a filter, but it is also a factory. It produces a protein called Alpha-1 Antitrypsin (AAT), which usually travels to the lungs to protect them from damage. In patients with this genetic deficiency, the liver produces misfolded versions of this protein.
These proteins get stuck inside the liver cells, causing physical stress and scarring (cirrhosis). While some patients develop lung issues, many others experience liver scarring without ever touching a drop of alcohol. In today’s modern landscape, we are seeing exciting progress in silencing the genes responsible for these broken proteins, which could prevent the liver from becoming overwhelmed.
Wilson’s Disease: The Copper Overload
Copper is vital for our nerves, but like anything in the body, balance is key. Normally, the liver acts as a gatekeeper, flushing out any extra copper through bile. In Wilson’s Disease, a genetic glitch breaks that flushing mechanism.
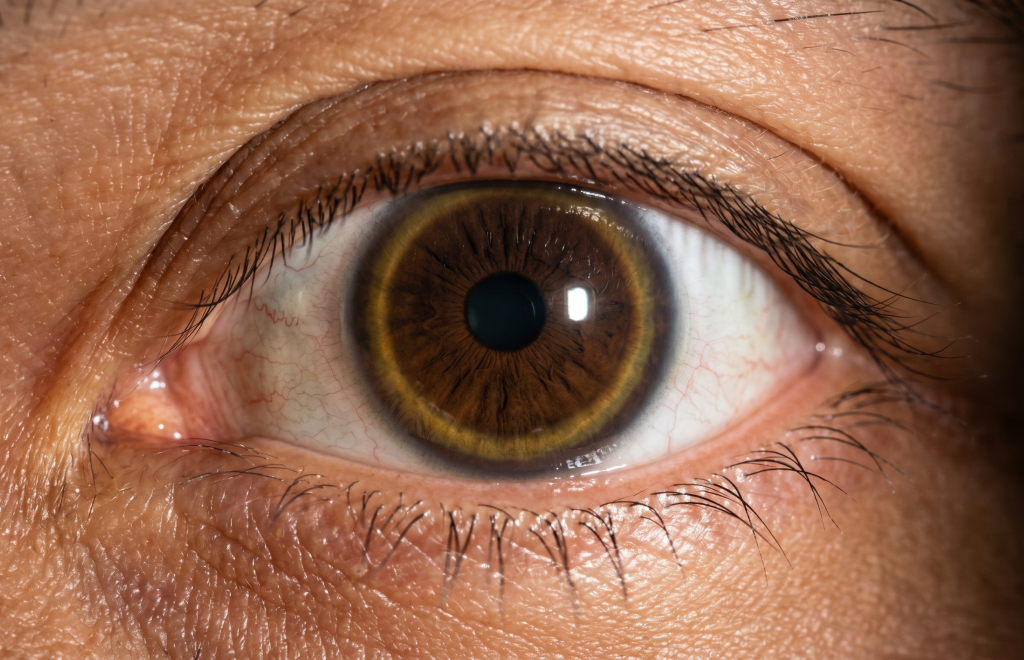
The copper begins to pile up, first in the liver and then in the brain and eyes. Physicians often look for a very specific sign called the Kayser-Fleischer ring, a circle around the iris of the eye. If this symptom is caught early, physicians can use chelating medicines that act like a magnet to pull the copper out of the body.
Primary Biliary Cholangitis (PBC): The Internal Itch
Primary Biliary Cholangitis is an autoimmune condition, meaning the body’s own defences mistakenly attack the small bile ducts within the liver. When these drainage ducts are damaged, bile—which we need to digest fats—leaks and builds up in the liver.
Women are more frequently affected by PBC. The most tell-tale symptom is not pain, but an intense, bone-deep itch that is often worse at night. For years, we only had one main treatment, Ursodeoxycholic acid (UDCA), but as of today, new medications like elafibranor have been approved. These drugs help the liver manage bile more efficiently and, crucially, provide significant relief from that debilitating itch.
A patient describes their symptoms before PBC diagnosis in the following reddit post:
Comment
byu/Unique_Ad_4271 from discussion
inLiverDisease
Primary Sclerosing Cholangitis (PSC): A Path of Scarring
While PBC affects the tiny pipes, Primary Sclerosing Cholangitis (PSC) attacks the larger ‘highways’ of the bile duct system. Inflammation causes these ducts to develop tough scar tissue, making them narrow and blocked. This is frequently seen in patients who also struggle with inflammatory bowel diseases like ulcerative colitis.
PSC is a challenging condition because it can lead to repeated infections and increases the risk of certain cancers. However, the landscape is shifting. Researchers are now testing synthetic bile acids, such as nor-ursodeoxycholic acid, which show promise in reversing some of the scarring.
“I got tired very easily and could not do things productively.”, described Ryan Lim, a PSC patient interviewed by The Straits Times. “I was also prone to falling sick often,”
Alagille Syndrome: A Shortage of Channels
Alagille Syndrome is a rare genetic puzzle usually diagnosed in childhood. These children are born with far fewer bile ducts than a healthy liver requires. Without enough bile ducts, bile accumulates rapidly, leading to jaundice (yellowing of the skin) and severe growth delays.
For a long time, the only solution for severe cases was a liver transplant. However, we now have specialised transporter inhibitors that help the body redirect bile acids through the kidneys instead. This simple shift in biology has been a game-changer for many families, reducing the need for surgery and allowing children to live much more comfortable lives.
Why ‘Rare’ Should Not Mean ‘Ignored’
In the medical community, most look for the common things first. But for those living with these rare liver diseases, they are often overlooked. If you have symptoms that do not quite fit the usual mould—persistent fatigue, skin that will not stop itching, or a family history of liver trouble—do not be afraid to ask for a deeper look.
From genetic testing to new targeted therapies, hospitals are increasingly more well-equipped to manage these conditions better than ever before. Knowledge is the most powerful tool we have to ensure that rare does not mean untreatable.
References:
- American Association for the Study of Liver Diseases. (2023). Practice guidance on primary sclerosing cholangitis and cholangiocarcinoma.
- American Liver Foundation. (2025). Alpha-1 antitrypsin deficiency
- Cruz, P. E., Mueller, C., Cossette, T. L., Golant, A., Tang, Q., Beattie, S. G., Brantly, M., Campbell-Thompson, M., Blomenkamp, K. S., Teckman, J. H., & Flotte, T. R. (2007). In vivo post-transcriptional gene silencing of alpha-1 antitrypsin by adeno-associated virus vectors expressing siRNA. Laboratory Investigation, 87(9), 893–902.
- European Association for the Study of the Liver. (2024). Clinical practice guidelines: The diagnosis and management of patients with primary biliary cholangitis.
- European Association for the Study of the Liver. (2025). Clinical practice guidelines on the management of Wilson’s disease.
- Khalik, S. (2024, April 2). Body against liver: Teenager overcomes rare autoimmune condition after transplant. The Straits Times.
- Liver Foundation Australia. (2026). Alpha-1 antitrypsin deficiency: Liver symptoms and management.
- Mayo Clinic. (2025). Wilson’s disease diagnosis and management.
- National Institute of Diabetes and Digestive and Kidney Diseases. (2024). Alagille syndrome.
- PSC Support UK. (2026). Research roundup: Norucholic acid trials.
- U.S. Food and Drug Administration. (2024). FDA grants accelerated approval to Iqirvo (elafibranor) for PBC.