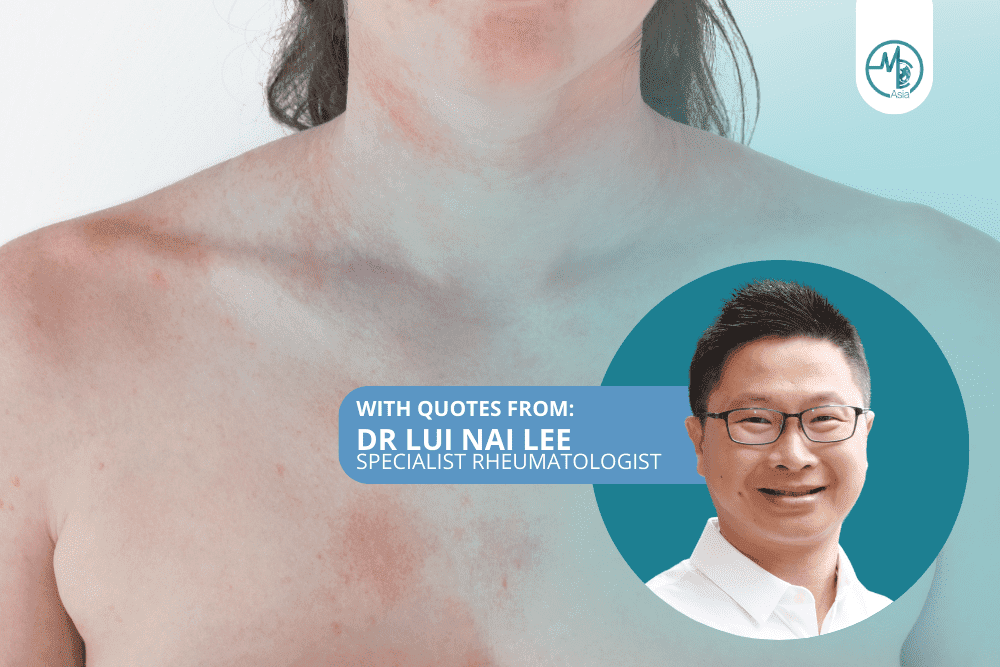
Lupus is a term that has graced many headlines, but the nuances of this autoimmune disorder remain enigmatic to many.
A complex condition, lupus requires a deep understanding to debunk myths and shed light on realities. Dive with us into the world of lupus as we unravel its mysteries, from causes and symptoms to management techniques with Dr Lui Nai Lee, a specialist rheumatologist and founder of Lui Centre for Arthritis & Rheumatology.
Lupus is often called the ‘disease of a thousand faces’ due to its varied manifestations. How do you approach diagnosing such a complex disease, and what are the typical presenting symptoms?
Dr Lui: It is indeed true that Lupus may be difficult to diagnose. This is due to its varied manifestations and occasionally very non-specific symptoms. For example, some patients only presenting symptom is fatigue!
Typical presenting symptoms include fatigue, recurrent low-grade fever & rashes at sun-exposed areas of the skin. They also include hair loss, oral ulcers, and muscle and joint pains.
Blood test evaluation may be the key to diagnosing Lupus in patients with non-specific symptoms and signs. We would usually assess the blood count, as some patients may suffer from anaemia or low white cell or platelet count. The other vital markers include the inflammatory markers erythrocyte sedimentation rate (ESR) and C-reactive protein, serum complements and autoimmune markers anti-nuclear antibody (ANA) and the anti-double stranded DNA.
Given the multisystem nature of the condition, how do you coordinate care with other specialists for comprehensive patient management?
Dr Lui: Rheumatologists are usually the primary carer for Lupus patients. However, some Lupus patients may have very complex issues requiring a multi-disciplinary team for their care. For example, Lupus patients may require consults with a Cardiologist due to heart issues and Nephrologist consults due to lupus nephritis. The Rheumatologists would set up the link with the other specialists and work together for better outcomes for the patient.
With emerging treatments and therapeutic strategies, what’s on the horizon for improving the management of lupus patients?
Dr Lui: One of the issues in treating Lupus is its’ complex and heterogeneous nature. For example, two patients with Lupus in the same family may have very different disease manifestations and responses to the same treatment and clinical outcomes. Over the years, genome-wide association studies (GWAS) have significantly improved our understanding of the genes and the immune mechanisms involved in Lupus. Based on this knowledge, scientists created and experimented with new therapies targeting different parts of the mechanism. This is with the hope to achieve better control of Lupus in some patients.
How do you address the challenges of treating patients of reproductive age, especially concerning pregnancy and family planning?
Dr Lui: The challenge is getting Lupus under control in patients of reproductive age. Some patients may be reluctant to consume certain medications due to possible side effects and possible teratogenic effects on the foetus should they get pregnant while consuming the medications. However, doing so may, more often than not, delay recovery.
The delayed recovery to a minimal disease activity state would mean that Lupus patients have to delay their planned pregnancies. More worryingly, without stronger medications, the delayed recovery may sometimes lead to the progression of disease to a more aggressive state. This causes further frustration and stress to the patient. Lupus patients should be in a minimal disease activity state for several months before conception to avoid complications of lupus pregnancy.
Dr Lui Nai Lee is a specialist rheumatologist at Gleneagles Medical Centre, Singapore. He manages autoimmune diseases such as Lupus, connective tissue diseases such as scleroderma, vasculitis (inflammation of blood vessels), Sjogren’s syndrome, inflammatory muscle diseases and various arthritic conditions and soft tissue rheumatism.