Discover how the National University of Singapore’s groundbreaking study revolutionises the treatment of pneumonia in ICU patients, showing that shorter courses of antibiotics are equally effective.
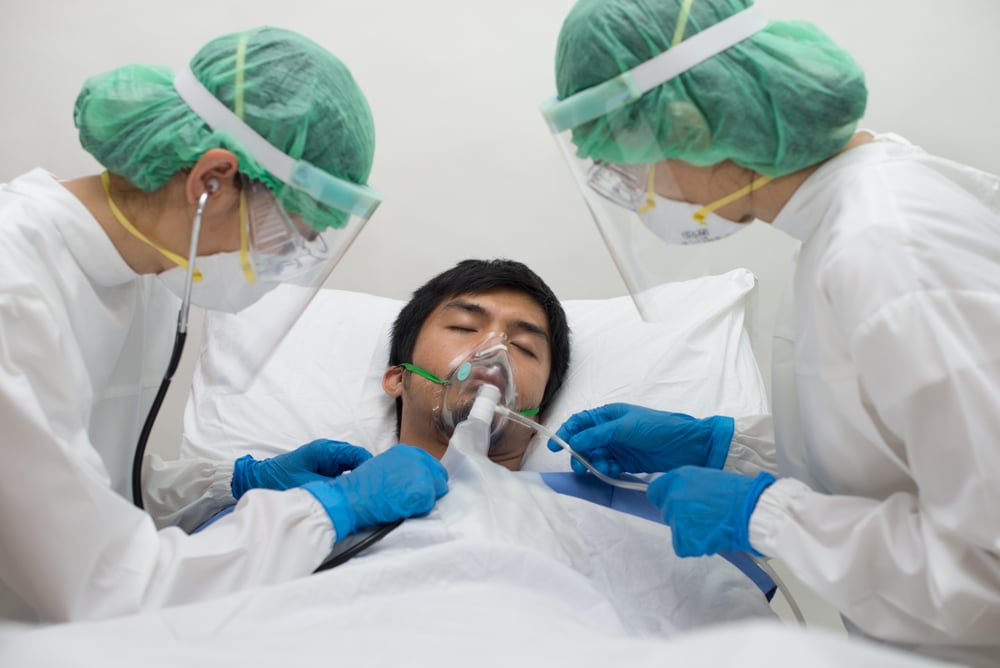
Ventilator-associated pneumonia (VAP) is a significant concern in intensive care units (ICUs), often necessitating prolonged antibiotic treatments. Challenging this standard practice, the National University of Singapore (NUS) conducted the “REducinG Antibiotic tReatment Duration for Ventilator-Associated Pneumonia” (REGARD-VAP) trial. This landmark study introduces a pivotal change in treating ICU pneumonia, suggesting that shorter antibiotic courses, tailored to individual patient responses, could be just as effective as the traditionally longer treatments.
Trial Overview
This randomised controlled trial compared the effectiveness of shortened antibiotic treatment against the standard, longer-duration therapy for VAP. The study encompassed multiple ICUs in Nepal, Thailand, and Singapore and involved 460 patients suffering from VAP.
Participants were randomly split into two groups. One group received a short-duration antibiotic treatment of 3 to 5 days. The other followed the longer, traditional treatment of at least 8 days. The main goal was to see if the shorter regimen was as effective in preventing death or pneumonia recurrence within 60 days, compared to the standard treatment.
Patient Selection and Methodology
In the REGARD-VAP trial, the selection of participants was meticulous, focusing on adult patients in ICUs who had been on mechanical ventilation for at least 48 hours and exhibited symptoms indicative of VAP. These symptoms included elevated body temperature, changes in white blood cell count, and new onset of respiratory issues, among others.
Once identified as potential candidates, patients underwent daily evaluations. The trial’s unique approach was to adjust the duration of antibiotic treatment based on each patient’s clinical response. For those in the short-duration treatment group, antibiotics could be discontinued as early as day 3 if respiratory cultures were negative, extending to day 5 for positive cultures. In contrast, the standard treatment group received a minimum of 8 days of antibiotics, as determined by their attending physicians.
This methodology not only allowed for a tailored treatment approach, responding to individual patient needs, but also set the stage for a potentially significant shift in ICU antibiotic treatment protocols for VAP.
Results and Implications
The REGARD-VAP trial’s findings have profound implications for medical practice, particularly in ICU settings. The study demonstrated that the shortened antibiotic treatment was just as effective as the standard, longer course in treating ventilator-associated pneumonia. This was evidenced by similar rates of death or pneumonia recurrence within 60 days across both patient groups.
A significant outcome of the trial was the reduction in antibiotic side effects. In the shortened treatment group, the incidence of side effects decreased dramatically from 38% to 8%. This reduction enhances patient comfort and safety but also lessens the burden on healthcare resources.
Furthermore, the trial’s results contribute to the global fight against antimicrobial resistance (AMR). By reducing the duration of antibiotic use, the trial supports efforts to diminish the risk of developing resistant bacterial strains. This is particularly important in the context of ICU care, where the emergence of multidrug-resistant organisms is a growing concern.
The REGARD-VAP trial, therefore, not only showcases a successful instance of optimising antibiotic use in critical care but also highlights the importance of personalised treatment strategies in improving patient outcomes.
Key Insights from the REGARD-VAP Trial
The trial represents a pivotal change in how ventilator-associated pneumonia is treated in ICU patients. The study’s revelation that shorter antibiotic courses can match the efficacy of traditional longer treatments paves the way for a more personalised approach to medical care.
This shift towards shorter antibiotic regimens offers several advantages. It minimises side effects for patients, a critical factor in improving their comfort and recovery experience. Equally important is its role in combating antimicrobial resistance.
By reducing antibiotic usage duration, the trial aligns with global efforts to prevent the rise of resistant bacterial strains. The study’s approach implies a more resource-efficient treatment methodology for VAP, beneficial in varied healthcare environments. The REGARD-VAP trial findings encourage a reevaluation of standard treatment protocols, advocating for antibiotic stewardship and responsive patient care.
References
- Less is more – shortened antibiotic treatment for ventilatorassociated pneumonia in ICU patients just as effective as standard course. (2024, January 26). National University of Singapore. https://medicine.nus.edu.sg/wp-content/uploads/2024/01/MEDIA-RELEASE_REGARDVAP-clinical-study-26JAN2024-FINAL.pdf
- Mo, Y., West, T. E., MacLaren, G., Booraphun, S., Li, A. Y., Kayastha, G., Lau, Y. H., Chew, Y. T., Chetchotisakd, P., Tambyah, P. A., Limmathurotsakul, D., & Cooper, B. (2021, May 1). Reducing antibiotic treatment duration for ventilator-associated pneumonia (REGARD-VAP): a trial protocol for a randomised clinical trial. BMJ Open. https://doi.org/10.1136/bmjopen-2021-050105