Though it affects millions of people worldwide, sickle cell disease is still relatively unknown to many. As such, World Sickle Cell Disease Day is observed on the 19th of June every year to raise awareness about this condition internationally. Read on to find out more about this blood condition that is affected by your genes.
What Is Sickle Cell Disease (SCD)?
Sickle cell disease (SCD) is a hereditary blood disorder that affects the oxygen-carrying protein, haemoglobin (Hb), in red blood cells (RBC).
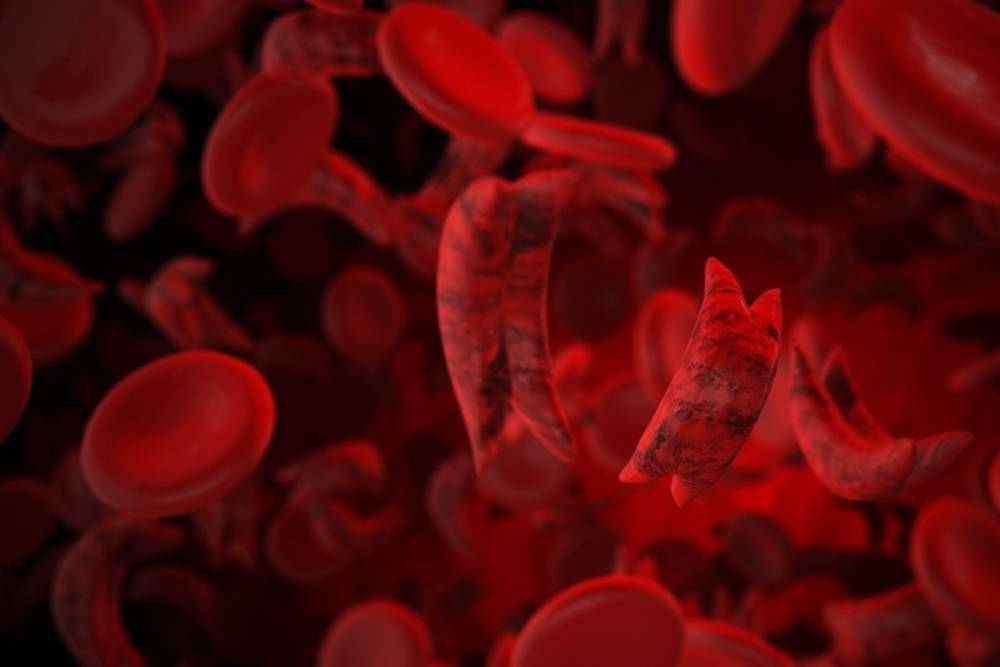
In a healthy person, RBCs with normal Hb are round and flexible, passing through small blood vessels easily, and delivering oxygen to tissues. In persons with SCD, RBCs with abnormal Hb are shaped like a sickle or crescent, are stiff and sticky, and thus get trapped easily in the small blood vessels. This obstructs the flow of oxygenated blood, leading to fatigue, pain and complications like end organ damage or even disability and death.
What causes Sickle Cell Disease?
A person will be born with SCD only if two genes are inherited—one from the mother and one from the father.
A person who inherits just one gene is healthy and said to be a “carrier” of the disease. If a carrier has a child with another carrier, there is a 25 % chance of having a child with SCD.
What are the symptoms of Sickle Cell Disease?
Anaemia
A healthy red blood cell lives for around 120 days. In people with SCD, the sickle cell lives for only 10 to 20 days and breaks down easily. When this happens, there is a shortage of oxygen-carrying red blood cells in the body resulting in anaemia, which may manifest as fatigue, dizziness and breathlessness.
Pain
A person with SCD may experience pain in different parts of the body like hands, legs, back and chest, depending on the location of blockage by sickled RBCs. E.g. Acute chest syndrome occurs when sickled cells stick together and block the flow of oxygen in the tiny vessels in the lungs. Symptoms resemble pneumonia and can include sudden fever and a violent cough besides pain.
The intensity and frequency of pain in SCD varies from person to person. Some might experience chronic pain and swelling due to joint damage and ulcers.
Frequent infection
The spleen helps to filter blood, fighting infections and removing old RBCs. Obstruction of blood vessels in the spleen by sickled RBCs and pooling can cause it to become enlarged. The spleen may become scarred and damaged. Because of this, the chances of contracting infections from bacteria like Haemophilus and Streptococcus are very high.
Stroke
This is another sudden severe complication of SCD. The sickled cells can block the major blood vessels that supply the brain with oxygen, causing brain damage, manifesting as numbness, weakness, paralysis, confusion, trouble walking and talking etc. After the first stroke, chances of recurrence are high.
Vision problem
If the tiny blood vessels that supply blood to the eye get blocked by sickle cells, the retina is damaged, thus affecting the vision of the person.
Delayed growth
Healthy and oxygenated blood packed with nutrients are highly essential for the normal growth of a person. In the absence of proper blood flow in the body, the growth of children and puberty may be delayed.
How to diagnose Sickle Cell Disease?
In developed countries like the USA, SCD screening is done as part of routine newborn screening tests.
India accounts for 15% of SCD worldwide. However, there is currently no neonatal screening programme for this condition. Diagnosis is done based on the symptoms of each person.
Different types of blood tests are conducted to diagnose SCD. Sometimes blood count will reveal an abnormal Hb level that points to SCD. Blood films might show an irregular shape of RBC which is the root cause of SCD. Haemoglobin electrophoresis measures Hb levels and looks for abnormal types of Hb; it can determine if a person is a carrier of sickle cell, or has any of the diseases associated with the sickle cell gene.
If either of the parents are diagnosed with SCD, the unborn baby is also tested by collecting the fluid from the mother’s womb. Testing before birth can be done as early as 8 to 10 weeks into the pregnancy.
What are the treatments available for Sickle Cell Disease?
The treatment for this condition mainly aims at reducing pain and preventing complications. Pharmacological and non-pharmacological treatment options are available for SCD.
Pharmacological treatment: Medications and Procedures
Hydroxyurea
Hydroxyurea helps to reduce pain crises, SCD complications e.g. acute chest syndrome and organ damage, hospitalisation and need for blood transfusion. However, it is not recommended for pregnant women as it can increase the chances of infection.
L-glutamine oral powder (EndariTM)
This is indicated in SCD patients ≥5 years of age to reduce pain related to the condition.
Crizanlizumab
This reduces the number of pain crises experienced by adults and children ≥16 years of age with SCD. It is given through the vein, helps prevent blood cells from sticking to blood vessel walls, thus preventing blood flow blockage, inflammation, and pain.
Voxelotor
This oral medicine lowers the risk for anaemia for adults and paediatric patients ≥12 years of age with SCD. It prevents RBCs from forming the sickle shape and binding together, decreasing the destruction of some RBCs, also improving blood flow to organs.
Penicillin
Penicillin is an antibiotic which may be given to both kids and adults to ward off infection like pneumonia, which can be life threatening for people with SCD.
Stem cell transplant
This method is otherwise known as bone marrow transplant. In this method, the bone marrow affected by the disease is replaced with a healthy bone marrow. The bone marrow is normally taken from a matched donor like a sibling.
Blood transfusion
This involves extracting RBCs from the blood of a donor and then injecting into the patient’s body. This increases circulation of normal RBCs which eventually improves oxygen and nutrient supply in the body.
Folate
Bone marrow requires folic acid and other vitamins for producing healthy RBCs. These may be obtained through a well-balanced diet or eating supplements.
Vaccinations
Get all recommended vaccines e.g. pneumococcal vaccine, the annual flu shot to prevent infections.
Non-pharmacological treatment: Lifestyle Tips
Stay hydrated
It is recommended to drink a minimum of eight glasses of water a day. Hydration helps to promote good blood flow and prevent RBCs from sickling and sticking together. It is thus important to replenish fluids especially with sweating due to heat or exercise. Avoid excessive caffeinated beverages and alcohol which may cause dehydration.
Adopt healthy habits
Exercise regularly without over-exertion, eat a well-balanced diet, quit smoking and get sufficient rest to maintain overall health as this helps to bump up immunity.
Conclusion
SCD is a lifelong condition. Early diagnosis is important in managing symptoms and preventing complications. Apart from medication and lifestyle changes, being well informed about the condition and having a good support group can help sufferers lead full, active lives.