The previous article on diabetic foot infection covered the symptoms, causes and types of diabetic foot infection. In this article, you will find 5 useful tips on how to prevent diabetic foot infection and 5 ways it is usually treated.
PSA: Medical Channel Asia (MCA) is now on Telegram! Join us here https://t.me/MedicalChannelAsia for daily reads and the latest updates at your fingertips!
5 Tips to Prevent Diabetic Foot Infection
1. Regular Foot Examinations With Your Doctor
If you have diabetes, you should visit your doctor or podiatrist to do a foot examination at least once a year. As a general rule, if you have type 2 diabetes, you should start the foot examination at the point of diagnosis. In comparison, if you have type 1 diabetes, you should begin your annual foot examination by your doctor 5 years after diagnosis. This can help to prevent diabetic foot infections from developing early.
If you have risk factors for diabetic foot ulcers such as previous episode(s) of foot ulcers, you should go for a foot examination more frequently. During your visit to the doctor, he or she would check the blood flow and sensation in your feet. By doing this, if there are any problems relating to your feet, your doctor can detect them right away and give you timely and proper treatment.
2. Daily Self Examination Of Your Foot
You can also self-examine your feet daily, paying more attention to areas between the toes and at the bottom of your feet. If you notice any broken skin, ulcer, blister, callus or redness on your feet, do see your doctor for further examination.

If you notice any pain, burning, tingling or numbness in your feet, take note of the frequency and severity. Inform your doctor and let them run further checks. Doctors may use a special device called a tuning fork to check if you can sense vibration in your foot and toe joints. This can help to determine if there is any nerve damage around that area.
3. Proper Foot Care
Avoid activities that can increase your risks of foot injuries like walking barefoot, going for pedicures where they cut your cuticles, or using a heating pad on your feet. You should also wear cotton socks that fit loosely and avoid tight-fitting shoes. When you trim your toenails, you should trim them straight across instead of cutting them down the sides or cutting them too short. If you notice any ingrown toenails, see your doctor or podiatrist for treatment.
4. Good Sugar Level Control
Having your blood sugar level under a good control and close to the target your doctor set for you would reduce the risk of poor blood circulation and nerve damage. This reduces the risk of diabetic foot complications.
5. Stop Smoking
Smoking causes problems for your heart and blood vessels. Smoking can also reduce blood circulation to your feet. By quitting smoking, it would improve your overall health and reduce the risk of diabetic foot complications.
You can use smoking cessation aids like nicotine replacement therapy (NRT). This comes in the form of gums, patches or lozenges. NRT helps to reduce the unpleasant withdrawal effects when you stop smoking, such as irritability, frustration, anger, anxiety, difficulty concentrating, restlessness, depression, difficulty falling or staying asleep, and nicotine craving. Doing so, helps you quit smoking more easily.
5 Ways to Treat Diabetic Foot Infection
The goal of treatment is always to preserve a functional limb. Here are some methods that your doctor might use to treat your infection.
1. Antibiotics
If your foot ulcer is infected, your doctor would prescribe you antibiotics. The type and duration of antibiotics chosen for you would depend on the depth and severity of your foot infection. If you have a mild infection, you would most likely be given oral antibiotics to complete. For severe infections, you might have to be hospitalized, as you may require the use of intravenous antibiotics (antibiotics administered directly into your bloodstream, bypassing the gut).
2. Debridement
In cases of superficial ulcers, your doctor might do debridement for you. Debridement means using a scalpel or scissors to clean the ulcer and remove the dead skin and tissue. Debridement is important for ulcer healing especially if dead skin and tissue are present.
3. Dressings
After debridement, your doctor would cover the area with a dressing to keep it clean. Dressings can give protection to the wound, promote wound hydration and/or prevent excess moisture on the wound. Some dressings have antimicrobial agents that can help to prevent infection and promote wound healing.
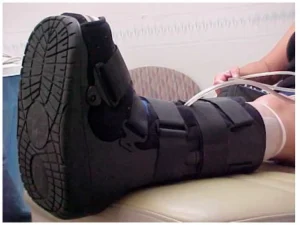
4. Reduction of Pressure on Foot Ulcer
If your foot ulcer is pressure-related, your doctor might suggest methods to reduce the pressure from the foot ulcer. For example, total contact casts (padded fibreglass or plaster shell), removable cast walkers (prefabricated brace), and prescriptive shoes with orthotic inserts or bedrest are recommended for offloading the pressure on your foot ulcer.
5. Surgery/ Revascularisation
If you have a severe infection, you mustn’t delay surgical treatment. Surgical excision of all dead and infected bone is recommended if the infection has penetrated the bone. As a last resort, doctors might consider amputation. Minor involvement of a digit can be treated safely with amputation of the affected digit. If arterial supply to the foot is compromised, your doctor might recommend revascularisation (also known as angioplasty or bypass grafting) to achieve wound healing and avoid amputation.
Conclusion
After your diabetic foot infection has been treated and the ulcer has healed, it is important to note that there is still a risk of recurrence. Therefore, remember to do daily self-examination of your foot and go for your annual foot check-ups so that you can remain ulcer-free, hospital-free and activity-rich.

