Treatments for Benign Prostatic Hyperplasia, or BPH, encompass a range of pharmacologic and surgical options. Technological advancements in surgical procedures in recent years have introduced Minimally Invasive Surgical Therapy (MIST) techniques, offering both patients and clinicians another treatment option for this common condition.
Dr Lee Fang Jann, a urologist from Urodoc Singapore, has a special interest in minimally invasive prostate enlargement therapy. In this video interview, he summarizes minimally invasive surgical therapies (MIST) available, and how they play a role in BPH treatment.
What is a prostate?
The prostate is a gland that rests below the bladder and surrounds part of the urethra. It is usually about the size of a walnut. Its most important function is the production of ejaculatory fluid. Together with sperm cells from the testicles and fluids from other glands, semen is produced. During ejaculation, the muscle cells of the prostate contract to forcefully expel semen.
What is Benign Prostatic Hyperplasia / Hypertrophy (BPH)?
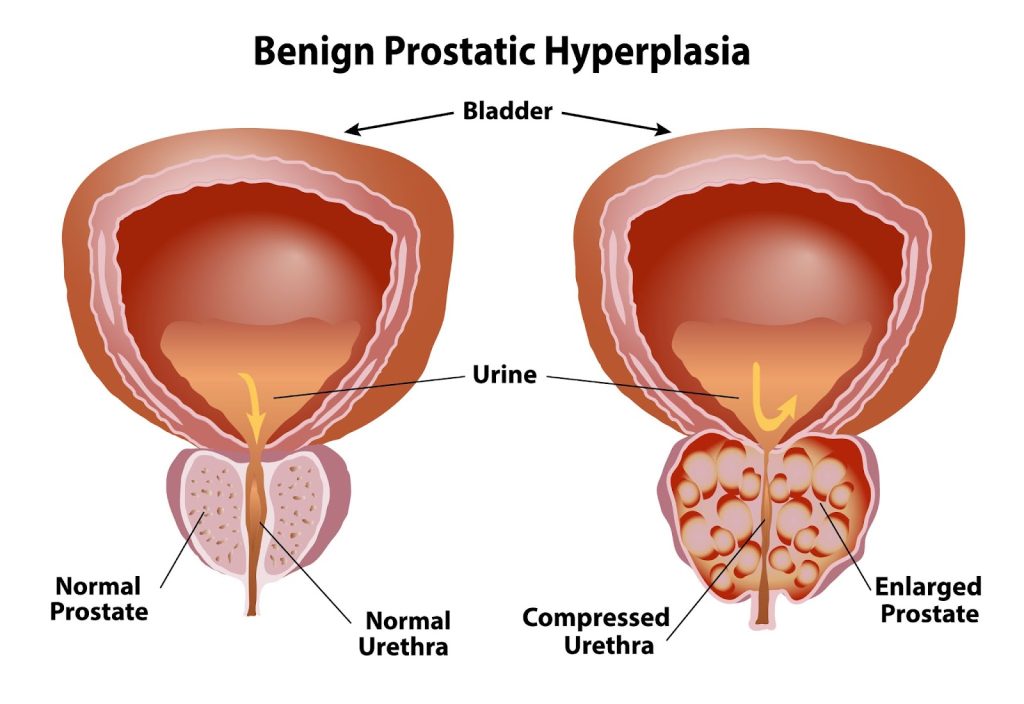
Benign Prostate Hyperplasia/Hypertrophy refers to the enlargement of the prostate gland. As the name suggests, BPH is not cancerous. BPH is neither linked to prostate cancer nor increases a man’s risk of developing prostate cancer. However, symptoms for BPH and prostate cancer can be similar.
BPH is a common problem which affects approximately 1 out of 3 men over 50 years old. The prevalence of BPH rises markedly with increased age, with the prevalence increasing to over 80% as men reach over the age of 80.
Why does the prostate enlarge with age?
The causes of BPH are not completely understood, but the male sex hormone testosterone is thought to play a role in the enlargement of the prostate. This is because the prostate is an androgen-dependent organ, requiring testosterone and the metabolite dihydrotestosterone (DHT) for growth and development. As testosterone is produced in the testes throughout a man’s life, they both stimulate cell growth in the prostate, thus it may continue to grow in size as the man gets older.
Besides ageing, other risk factors for BPH development include:
- Family history: If a blood relative such as a father or a brother suffers from BPH, one is more likely to also develop BPH.
- Other medical conditions: There are studies to show that diabetes, cardiovascular disease and erectile dysfunction are closely correlated with BPH.
- Lifestyle: Obesity is linked to an increased risk of developing BPH. On the other hand, regular physical activity is shown to improve prostate health and prevent BPH.
Minimally Invasive Surgical Therapy (MIST) for the treatment of BPH
There are many options available for treating BPH. The attending doctor would assess the patient’s condition to understand the most appropriate treatment for them,
For mild to moderate symptoms, the condition may be managed conservatively via active surveillance, or with pharmacotherapy. For more severe conditions which do not get sufficient relief from the use of medication alone, or if medication side effects are of concern, surgical options are available to give long-lasting relief.
Over the years, newer technologies have been developed to treat BPH that is minimally invasive. These procedures may include the use of tiny incisions or the use of tube-style instruments inserted through the urethra to access the prostate. Being minimally invasive, they can often do as a short outpatient procedure, and incur a shorter recovery time.
There are several types of MIST available for BPH. The option will depend on factors such as the size of the prostate, other health conditions, and one’s personal choice.
Prolieve®: Focused Microwave Heating with Pressurized Balloon Dilation Therapy
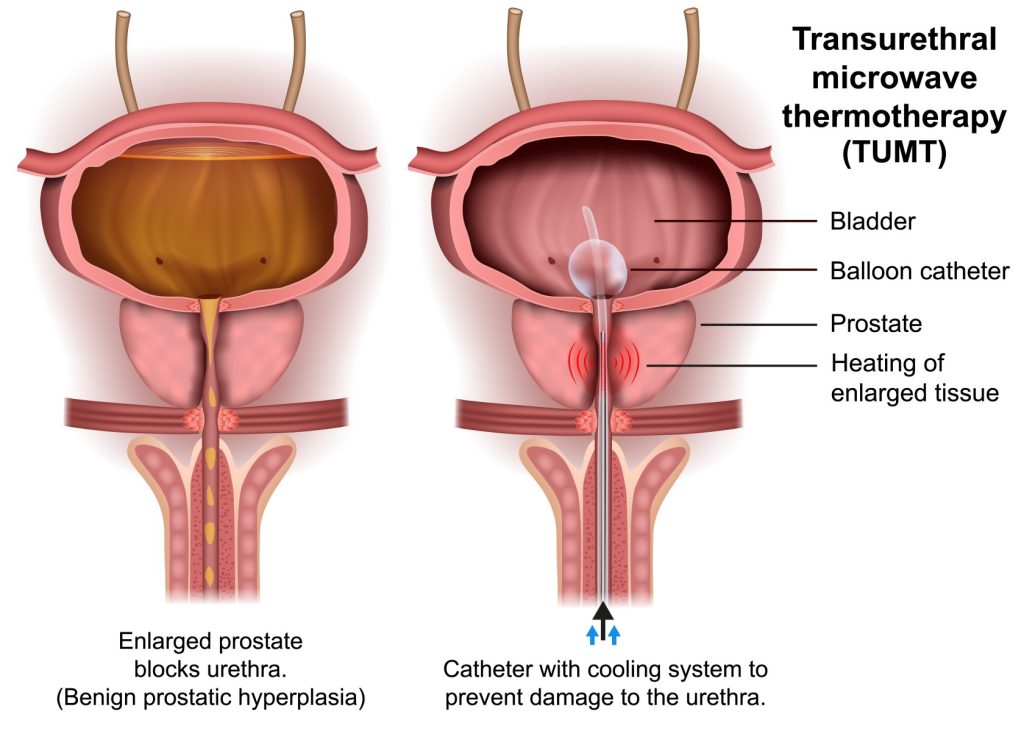
The Prolieve system combines Thermotherapy with Balloon Dilatation to open up the constricted urethra and compress the prostate. The procedure lasts about 45 minutes and can be done in-office.
Process:
- Local anaesthetic is applied to the tip of the penis. The patient may be given sedation for the procedure.
- A catheter is placed inside the bladder, guided via ultrasound. This catheter contains a dilation balloon with a special antenna.
- A temperature monitor is also inserted rectally to gauge the temperature of surrounding tissues and keep them within safe parameters.
- The balloon is inflated, expanding the prostate tissue and dilates the urethra much like a stent. At the same time, microwave energy is transmitted from the special antenna, providing heat to shrink the enlarged prostate tissues.
- Throughout the procedure, warm water is circulated inside the catheter to regulate the temperature and improve comfort.
How it works
The pressurized balloon expands, pushing apart the prostate tissue and immediately creates a wider passage for urine to pass through. The heat-treated tissue will have residual effects, subsequently shrink and disappear. Hence, the treatment can take up to a year to see improvement gradually.
UroLift®: Implants
Also known as Prostatic Urethral Lift (PUL), the Urolift procedure involves implants placed via a small scope passed through the urethra. These implants ‘lift’ the prostatic tissue, opening up the urethral channel without the need to remove any tissue via heating or cutting.
The procedure is typically performed under local anesthesia or sedation as day surgery, lasting only 5-10 minutes. Patients can return home on the same day without a catheter.
Rezūm: Water Vapor Therapy
As the name suggests, Rezūm Water Vapor Therapy works by injecting multiple 9-second bursts of precise doses of sterile water vapor (steam) through a cystoscope. When the steam comes into contact with prostate tissue, the thermal energy in the steam is released into the targeted tissue via convective heat transfer.
Over time, the body will absorb the treated tissue, shrinking the prostate. With the extra tissue removed, the urethra is no longer compressed, thus reducing BPH symptoms.
The procedure is typically performed under local anesthesia or sedation as day surgery, lasting only 5-10 minutes. However, a urethral catheter is required during the recovery process, lasting 5-14 days post-procedure.
Conclusion
The treatment landscape for BPH is evolving over the years, with the development of MIST procedures at the forefront. For patients who prefer to forego invasive surgery, looking for quick and effective therapies, with reduced downtime that also preserves sexual function, MIST procedures outlined above provide more options and an alternative to traditional pharmacotherapy and surgical procedures.
These MIST procedures are not without their limitations. There are selection criteria for these procedures, and not all prostates can be treated by MIST procedures. For instance, very large prostates, or patients who are suffering from BPH complications such as urinary retention or blocked kidneys may not be suitable candidates for MIST procedures. Instead, more invasive surgery may be warranted to treat the larger volumes of prostate tissue, and address complications.
If one is experiencing symptoms of BPH including urinary frequency, urinary urgency, nocturia (waking up at night to urinate), and hard time starting and stopping urination, it is important to consult a urologist to be evaluated. With the treatment options available, the urologist can help to individualize treatment for each patient’s condition.
This article is supported by an educational grant.