This article on Osgood Schlatter Disease first appeared on Physioactive Blog.

Has your child been diagnosed with Osgood Schlatter Disease? Well, fear not – it’s not as scary as it sounds!
What You Need to Know
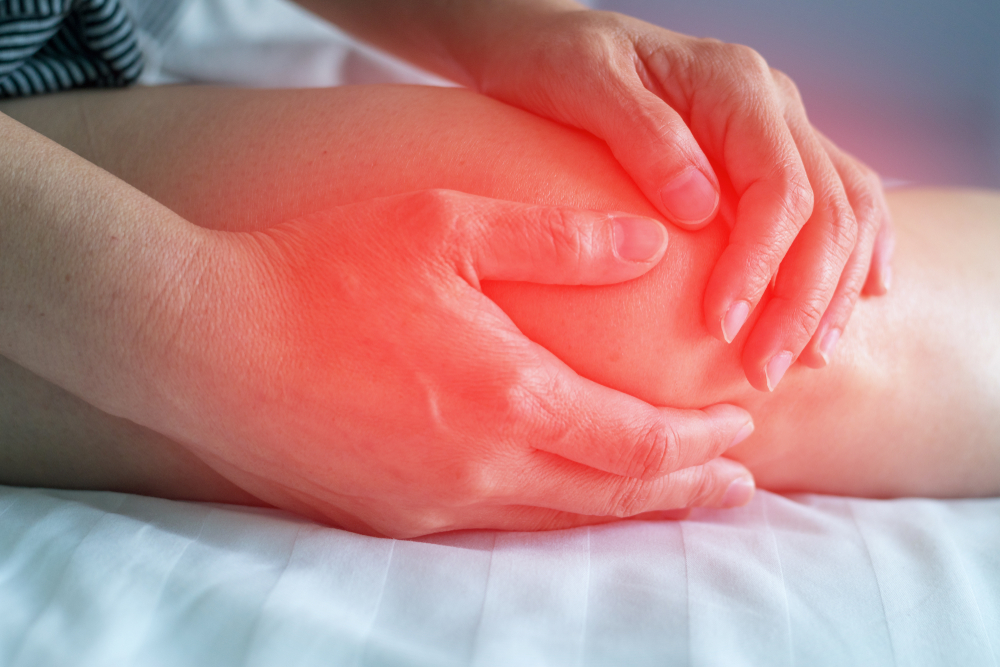
Osgood Schlatter Disease (OSD) is not a true disease, but an overuse injury of the knee. It is a common, temporary musculoskeletal condition that causes knee pain in older children and teenagers. It most often occurs during times when the bone is growing quickly, for example during the teenage growth spurt. OSD is more common in boys. In boys, it is usually reported between 12-16 years. In girls, this growth spurt occurs a little earlier between 11-15 years. Children who participate in running and jumping sports are at an increased risk of OSD (affecting 21%). Less active children are at lower risk (affecting 4%) but can also experience this problem. Pain is located very precisely so diagnosis is rarely a problem. Patients can point exactly to it – a tender bony bump at the top of their shinbone, below their knee. An x-ray is usually unnecessary.
Anatomy Explained
OSD is caused by irritation of the bone growth plate. While a child is still growing, these growth plates are in the form of cartilage rather than bone. The tendon from the kneecap (patella) attaches down to the growth plate in the front of the shin bone (tibia). The thigh muscles (quadriceps) attach to the kneecap, and when they pull on the kneecap, this puts tension on the patellar tendon. The patellar tendon then pulls on the shin bone, at the area of the growth plate. Cartilage is not as strong as bone, so high levels of stress can cause the growth plate to begin to hurt and swell.
While most children will develop OSD in one knee only, some can develop it in both knees. In almost every case, surgery is not needed. This is because the cartilage growth plate eventually stops its growth and fills in with bone when the child stops growing. The knee pain almost always stops once the child is finished growing, but symptoms may come and go during this period for 1-2 years after.
Sports and Movements
Any movements that involve bending and straightening of the knee can lead to tenderness at the point where the patellar tendon attaches to the top of the tibia. Activities that repeatedly place this stress on the knee, especially squatting, kicking, jumping or running, can cause the tissue around the growth plate to hurt and swell.
In some cases, your child may need to stop sporting activities for a short period, to allow pain levels and inflammation to settle down. Patients who do require a rest period usually do not need to avoid sports for a long time, and often relative rest is adequate. Relative rest means decreasing the intensity or frequency of your sporting activities but not stopping them completely. A physiotherapist can advise you regarding which of these would be most appropriate.
Physiotherapy Intervention
If your child is diagnosed with the condition, the first step would be to schedule in a physiotherapy appointment. A physiotherapist would typically begin with a baseline assessment of your child’s:
- Functional pain levels
- Range of motion (ROM)
- Lower limb strength
- Functional balance
Based on the assessment, the physiotherapist can design a targeted exercise program to effectively manage OSD. This may involve:
- Pain management: Massage and ice application can be used to loosen tight muscles, reduce pain and decrease inflammation. This can be particularly beneficial in the early phase when most painful.
- Stretching exercises: Many children with OSD have tightness in one or more muscle groups in their legs. This tightness can increase the pull on the patellar tendon and the area of pain. The physiotherapist may include hamstring stretches, quad stretches, and calf stretches to improve flexibility.
- Strengthening exercises: The restriction of movement during the recovery period can cause muscles to shorten and become weaker. This again may cause increased stress on the area of pain. The physiotherapist will include exercises aimed at strengthening the affected muscles such as the quadriceps, hamstrings, and hip muscles. Strengthening a knee that is painful can be difficult, so it is important to follow the strict instructions of your physiotherapist regarding increasing or decreasing the load of the exercise.
- Balance and coordination exercises: Some children with OSD experience impaired balance and coordination. To overcome this, your physiotherapist would teach balance exercises to improve balance and strength in the affected knee, hip, and ankle.
Passive treatments like heat, ice, or taping may feel good and help a little, but they do little to improve the underlying condition. Ultimately, the best treatment for OSD is an active physiotherapy rehab program. To speed up recovery, it always helps to have an informed exercise plan designed to improve mobility and strengthen and stabilise the knee. By working with a physiotherapist, your child is highly likely to recover quicker than sitting at home or on the sidelines.
—
This post has been written by Physiotherapist Liam Mc Ginley MSc, MCSP