Robotic-assisted gynaecological surgery is transforming women’s healthcare with less pain, faster recovery, and greater precision – so what does this mean for patients?
For many women, the idea of gynaecological surgery can bring to mind large incisions, prolonged hospital stays, and weeks – perhaps even months – of recovery. As it is, there was a time when procedures involving the female reproductive system used to require surgeons to physically expose organs to operate. This came at the cost of pain, scarring, and significant disruption to a patient’s life.
However, the advent of minimally invasive robotic technology has resulted in a dramatic change to this paradigm.
The operating theatre is no longer a place designated just for scalpels and sutures, but for high-definition cameras, robotic arms, and surgeons seated at consoles, guiding movements with remarkable precision. Minimally invasive robotic surgery is more than just a technological upgrade – it represents a shift in what it means to undergo surgery.
We spoke with Dr Sevellaraja A/L N. Supermaniam, an obstetrician and gynaecologist at Mahkota Medical Centre, to learn how this evolution is reshaping the future of gynaecological care.

The Core Concerns of Gynaecological Surgery
“When patients are told they may need gynaecological surgery, their concerns are often immediate and deeply personal,” said Dr Selva.
“Most centre around three key areas: pain, safety, and fertility.”
The thought of going through any type of surgery can be daunting, as we worry about discomfort and recovery, as well as any complications that can come about during and after a procedure.
When it comes to gynaecological surgery in particular, fertility is another emotional layer that can heighten anxiety.
“The question, ‘Will I still be able to get pregnant?’ is commonly raised, especially among those who wish to have children in the future,” he elaborated.
“Even when the procedure is minor, uncertainty about its impact on reproductive health can cause significant emotional distress.”
However, with the advancement of gynaecological surgery, many procedures now are minimally invasive, leading to less pain, shorter recovery periods, and safer, more predictable outcomes.
How Gynaecological Surgery Has Evolved
From highly invasive open surgeries to more precise, patient-friendly techniques, gynaecological surgery has gone through several transformations in the last few decades. The initiation of laparoscopy, used to diagnose and treat conditions such as endometriosis and ovarian cysts, marked one such turning point.
“Instead of large cuts, surgeons began operating through small “keyhole” incisions using a camera to guide the procedure. This approach significantly reduced trauma to the body,” explained Dr Selva.
It improved surgical outcomes and patient satisfaction overall, allowing patients to return to normal activities much sooner than before.
Hysteroscopy, which involves inserting a thin scope through the cervix, has further refined treatment options, particularly for conditions within the uterus.
“By allowing doctors to access and treat conditions without any external incision, it eliminated visible scars altogether. Many of these procedures can also now be done as day-care cases, meaning patients come in, undergo treatment, and go home on the same day. This would have been unthinkable in the past.
“Overall, these advancements have not only improved clinical outcomes but have also made gynaecological surgery far more patient-centric, reducing fear and enabling women to recover faster and with greater confidence.”
However, innovation in the realm of gynaecological surgery hasn’t stopped there. At present, there is an exciting development demonstrating significant potential in further alleviating the surgical experience for both patients and doctors: robotic-assisted surgery.
The Rise of Robotic Technology
According to Dr Selva, robotic-assisted surgery “represents another leap forward”.
During a procedure, the surgeon will sit at a console and control the robotic arms that are carrying out the operation in real-time.
“By combining the surgeon’s expertise with advanced technology, robotic-assisted surgery allows for more refined techniques while still maintaining the benefits of minimally invasive surgery, such as smaller incisions and potentially faster recovery.”
It grants several benefits for a surgeon, including:
- Improved vision via a high-definition, three-dimensional, magnified view of the surgical field, allowing greater clarity and visual detail even when normal anatomy is altered.
- More precise movements through “wristed” instruments that rotate in ways that mimic the natural motion of the human hand, enabling greater range of motion and enhanced stability.
- Greater suturing capabilities, especially in confined or complex anatomical spaces where vital organs and structures are closely positioned.
- Better ergonomics as the surgeon can operate from a seated console rather than standing for long hours in physically-demanding positions.
These advantages make robotic-assisted surgery especially important for difficult cases such as severe endometriosis, large fibroids requiring reconstruction, and deep pelvic surgery, or for patients with obesity where surgical access can be more challenging. These situations often involve distorted anatomy, limited working space, and a higher level of technical difficulty.
“In such situations, the technology allows for cleaner dissection, better preservation of surrounding organs, and greater surgical precision overall,” he stated.
Robotic-assisted surgery ultimately offers doctors more control and confidence in handling complex cases, helping them achieve better patient outcomes.
Adopting Japan’s hinotori™: A First in Malaysia
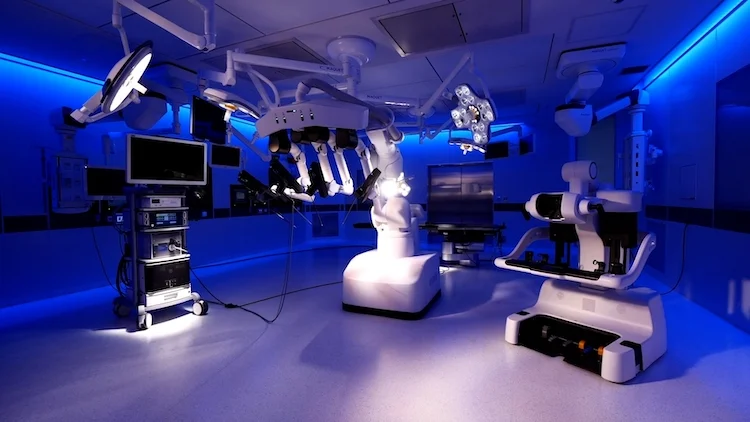
Recently, in a move towards expanding the field of robotic-assisted surgery, Mahkota Medical Centre became the first referral hospital outside of Japan to launch hinotori™, a cutting-edge robotic surgical system.
“It marks a first-in-Malaysia milestone for us, and we have also just recently completed over a hundred surgeries, which we are extremely proud about,” Dr Selva announced.
Despite hinotori™ being relatively new compared to other established robotic platforms, early experience already demonstrates its promise for procedures that require fine dissection, and careful handling of delicate structures. For instance, one key aspect that sets this system apart is its strong focus on precision and flexibility.
“The robotic arms are designed with a wider range of motion, allowing for more refined and controlled movements during surgery.”
The system provides greater access to tight anatomical areas and navigates limited spaces with ease.
“In addition, the compact design of the platform makes it more streamlined within the operating theatre, potentially improving workflow and efficiency.”
From a practical standpoint, another plus is in how the setup feels more intuitive, and the instrument movements are both smooth and responsive.
“This contributes to a more natural surgical experience, allowing the surgeon to focus on precision and technique.”
The Future of Gynaecological Care
With robotic-assisted surgery, greater precision, less trauma and speedier recovery may soon be expected features of gynaecological procedures.
“We are moving toward a more personalised approach to surgery, where treatment is tailored to each patient’s condition, anatomy, and reproductive goals. There is also a stronger emphasis on organ preservation, especially in women who wish to maintain fertility or avoid more radical procedures,” remarked Dr Selva.
Another important point he brought up is the increase in combination treatments.
“Surgery is no longer the only option. It can now be integrated with other modalities such as high-intensity focused ultrasound (HIFU) and medical therapy. This allows for more a comprehensive and less invasive management of complex conditions.”
Should I choose robotic surgery?
Even with the support of technological advancement, it is important to emphasise that a patient’s journey can still vary depending on their individual circumstances. As such, Dr Selva has one key advice for patients: ask questions.
“Understand why a particular approach is being recommended, explore alternative options, and make sure you know the potential risks and benefits. Avoid choosing a procedure simply because it uses the ‘latest technology’.”
Patients and doctors must choose the approach that best suits the individual condition to achieve the safest and most effective outcome.
Should you have any concerns, it is also part of a clinician’s role to address those fears with clarity and empathy. They can explain what the procedure involves, outline the safety measures in place, and discuss the expected recovery process.
“Ultimately, clear communication and patient education are essential. When patients understand what to expect, their anxiety is often reduced, allowing them to approach surgery with greater confidence and peace of mind.”
External References
- Cleveland Clinic. (2022, September 12). Hysteroscopy. Retrieved from: https://my.clevelandclinic.org/health/treatments/10142-hysteroscopy
- Cleveland Clinic. (2024, March 1). Laparoscopy. Retrieved from: https://my.clevelandclinic.org/health/procedures/4819-laparoscopy

