Benign prostatic hyperplasia is a condition where the prostate enlarges, and it affects most ageing men. Fortunately, with the advancement in treatment options, not all cases require surgery. Here is how newer treatments are changing the approach.
It usually starts insidiously: A weaker stream. A longer wait in the bathroom. Waking up once, then twice, then three times a night. For many men, these changes are brushed off as a normal part of ageing.
But for millions across Asia, these symptoms point to something far more specific: benign prostatic hyperplasia.
What is Benign Prostatic Hyperplasia (BPH)?
Benign prostatic hyperplasia (BPH) refers to the non-cancerous enlargement of the prostate gland, a condition that becomes increasingly common with age.
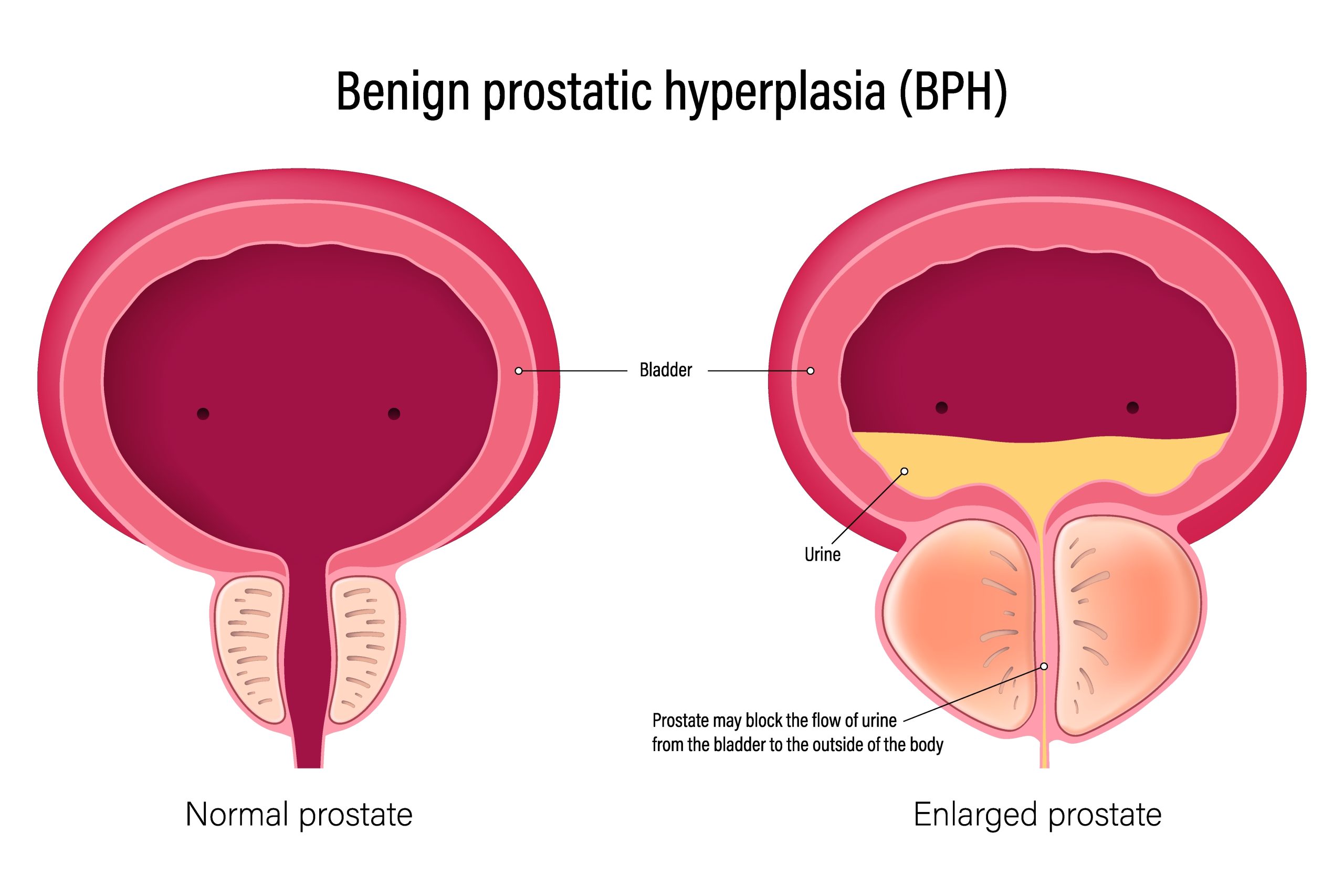
The prostate sits just below the bladder and surrounds the urethra – the tube that carries urine out of the body. As it enlarges, it can compress this passage, leading to urinary symptoms such as:
- Weak urine flow
- Difficulty starting urination
- Frequent urination, especially at night
- A sensation of incomplete emptying
In Singapore and across Southeast Asia, BPH is one of the most common urological conditions in ageing men. Studies suggest that around 50% of men in their 50s experience some degree of prostate enlargement. This rises to up to 80-90% in men over 80.
While not life-threatening, BPH can significantly affect quality of life – in particular sleep, daily routines, and even mental well-being.
The Gold Standard: Why Surgery Has Long Been the Answer
For decades, the most definitive treatment for moderate to severe BPH has been transurethral resection of the prostate (TURP).
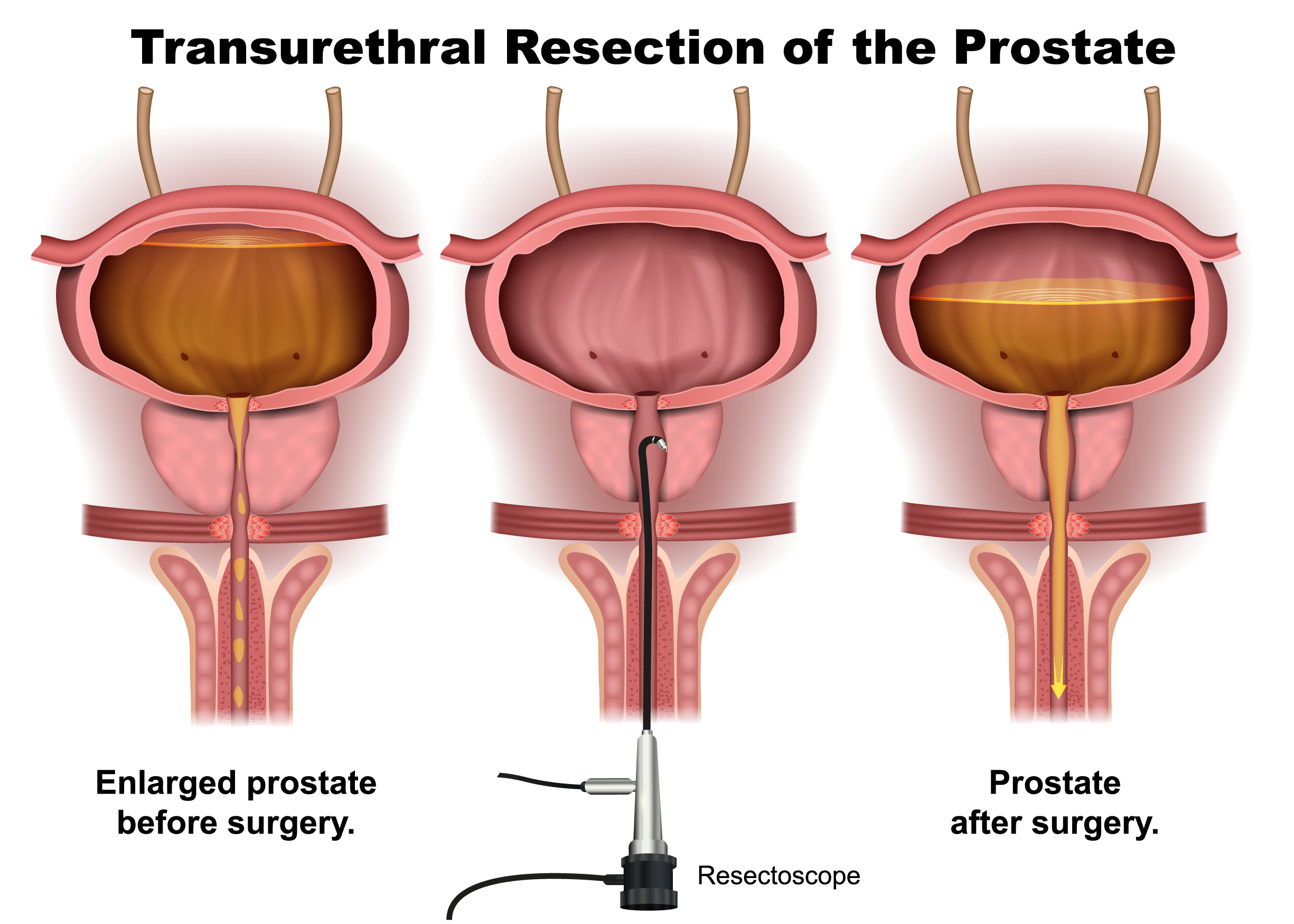
In this procedure, a surgeon inserts a resectoscope through the urethra and removes excess prostate tissue to relieve the obstruction.
TURP remains widely regarded as the gold standard for BPH because it provides significant and durable symptom relief, improves urine flow reliably, and has well-established long-term outcomes.
Risks of a TURP
While there are no visible skin incisions, TURP is still a form of surgery, and comes with its own set of risks and side effects.
The surgery is usually carried out under general anaesthesia, or regional anaesthesia, which means downtime for recovery. A urinary catheter will be required to manage swelling and maintain urinary output.
There are also potential risks, including bleeding, infection, and side effects such as retrograde ejaculation. For many men, especially those with milder symptoms or concerns about recovery and side effects, the risks to benefit ratio may not be the most favourable when it comes to the invasive TURP procedure.
Well, what if you could treat an enlarged prostate without cutting it out?
Three Ways to Treat an Enlarged Prostate Without Surgery
In recent years, a growing category of treatments has emerged, often referred to as Minimally Invasive Surgical Therapies (MIST). These approaches aim to relieve obstruction without removing prostate tissue surgically.
Here are three such options.
1. Prostatic Urethral Lift
The prostatic urethral lift works by physically pulling apart the enlarged prostate tissue, rather than removing it.
Small implants are placed within the prostate to retract the obstructing lobes, creating a wider channel for urine flow.
What makes this approach notable is that it:
- Does not involve cutting or heating tissue
- Can often be performed as a day procedure
- Has a lower risk of sexual side effects compared to traditional surgery
For patients concerned about preserving sexual function or avoiding more invasive procedures, this option has gained increasing attention.
2. Temporary Implantable Nitinol Device
Another approach uses a temporary device placed within the prostate to reshape it.
This device, made from a flexible metal alloy, is inserted into the urethra and left in place for a short period, typically 5 to 7 days. During this time, it gently expands and applies targeted pressure at specific points within the prostate.
Rather than removing tissue, it works by creating small, controlled channels within the prostate through sustained pressure, which leads to subtle remodelling of the urinary passage. Once the device is removed, these changes remain, allowing urine to flow more freely.
What makes this approach distinct is that it:
- Does not require permanent implants
- Does not use heat or cutting energy
- Can be performed in a clinic or day procedure setting, often under local anaesthesia
It is generally considered most suitable for men with moderate prostate enlargement and preserved bladder function, where anatomy allows for effective reshaping. This method is particularly appealing for patients seeking a reversible and non-permanent intervention.
3. Drug-coated Balloon Therapy
A newer approach combines mechanical dilation with targeted drug delivery to treat an enlarged prostate – much like heart procedures.
In this method, doctors insert a small balloon into the urethra and gently inflate it at the level of the prostate. This action widens the narrowed urinary channel, much like how angioplasty opens blocked blood vessels.
They also coat the balloon with a medication called paclitaxel, an agent that helps prevent tissue from growing back or re-fusing during healing. As they inflate the balloon, it delivers the drug directly into the surrounding prostate tissue, helping to stabilise the opening created by the procedure.
the treatment works in two steps:
- Mechanically opening the blocked passage
- Biologically maintaining that opening over time
Unlike traditional surgery, there is no cutting or removal of prostate tissue. The procedure is typically quick and minimally invasive, with no permanent implant left behind. For patients, this means the potential for rapid symptom relief with a relatively short recovery period.
Early data have shown encouraging improvements in urinary symptoms and flow rates, with durability extending beyond the initial treatment period. Side effects may include temporary incontinence or mild bleeding, but these are generally short-lived.
So, Which Option is Right for You?
BPH is no longer a condition with a one-size-fits-all solution.
Instead, it is increasingly managed as a spectrum, where treatment can be tailored – from medication to minimally invasive procedures, and finally to surgery when needed.
For many men, the conversation is no longer just whether to treat BPH, but how. And for that, the choice of treatment depends on several factors, including:
- Severity of symptoms
- Size and anatomy of the prostate
- Patient preferences, especially regarding recovery and sexual function
- Medical suitability for surgery
While TURP remains a highly effective and reliable option, these newer MIST therapies offer alternative pathways for patients who may not want (or need) traditional surgery.

