Though under-reported, back pain is quite common among adults. Studies have shown that 4 out of 5 adults encounter debilitating back pain which disrupts daily life at least once in their lifetime. Understanding what causes it, taking steps to prevent it, and how to manage it when it happens, is then crucial. Read on to find out more, or listen to an orthopaedic surgeon explain more at the bottom of the article.
Anatomy of the spine
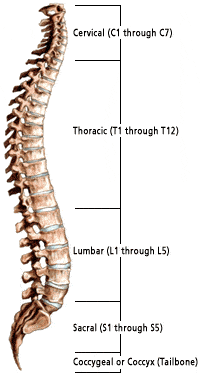
Before delving into back pain, it is helpful to understand the basic structure of the spine.
The spine is made up of 33 bones called vertebrae stacked on top of each other and is divided into 5 distinct regions.
- Neck area: cervical vertebrae (C1 to C7)
- Chest: thoracic vertebrae (T1 to T12)
- Region in your lower back: lumbar vertebrae (L1 to L5)
- The sacrum is a triangle-shaped bone which connects to the hips
- The coccyx or tailbone is found at the bottom of the spine.
The vertebrae form a tunnel or spinal canal through which the spinal cord runs. The spinal cord is a bundle of nerves that send messages from the brain to the body and vice versa. Between the vertebrae there are soft cushions called discs, which act as shock absorbers. Each disc has two parts: a soft, gelatinous inner portion (Nucleus Pulposus) and a tough outer ring (Annulus Fibrosus).
Classification of Back pain
Back pain can be classified based on the location affected.
Upper back pain
- The upper back comprises 12 bones or vertebrae (T1 to T12) which start at the base of the neck and go down to the bottom of the ribcage. It is called the thoracic spine. Our thoracic spine is not designed to withstand prolonged curving. Mild to intense pain in the neck and upper back is experienced by many people due to frequent bending forward while working on the computer or mobile. It occurs likewise in teenagers with long hours of screen time. These people usually feel increased tension after extended periods of sitting in a fixed position.
Lower back pain
- It is a pain in the last five vertebrae of the spine (L1 to L5) known as the lumbar spine, which is the part that bends inwards at the bottom. Improper stretching of this region causes lower back pain. The most frequent cause of lower back pain is sitting with a bad posture such as hunched position for a long time.
Causes of back pain
The COVID pandemic has seen a rise in the incidence of aforementioned posture-related back pain due to more people being cooped up at home watching television or playing video games for prolonged durations in less than ideal positions. Another significant factor stems from working on the computer for long hours, being desk-bound for most parts of the day.
Other common causes of back pain are a result of lifestyle:
- Smoking – toxins from tobacco prevent intervertebral discs from getting the nutrients they need to stay healthy and flexible. This accelerates their damage and degeneration which manifest as pain.
- Heavy weightlifting without proper technique
- Being overweight
- Sports injuries cause mechanical damage to the spine and consequent pain
Medical Conditions that cause Back Pain
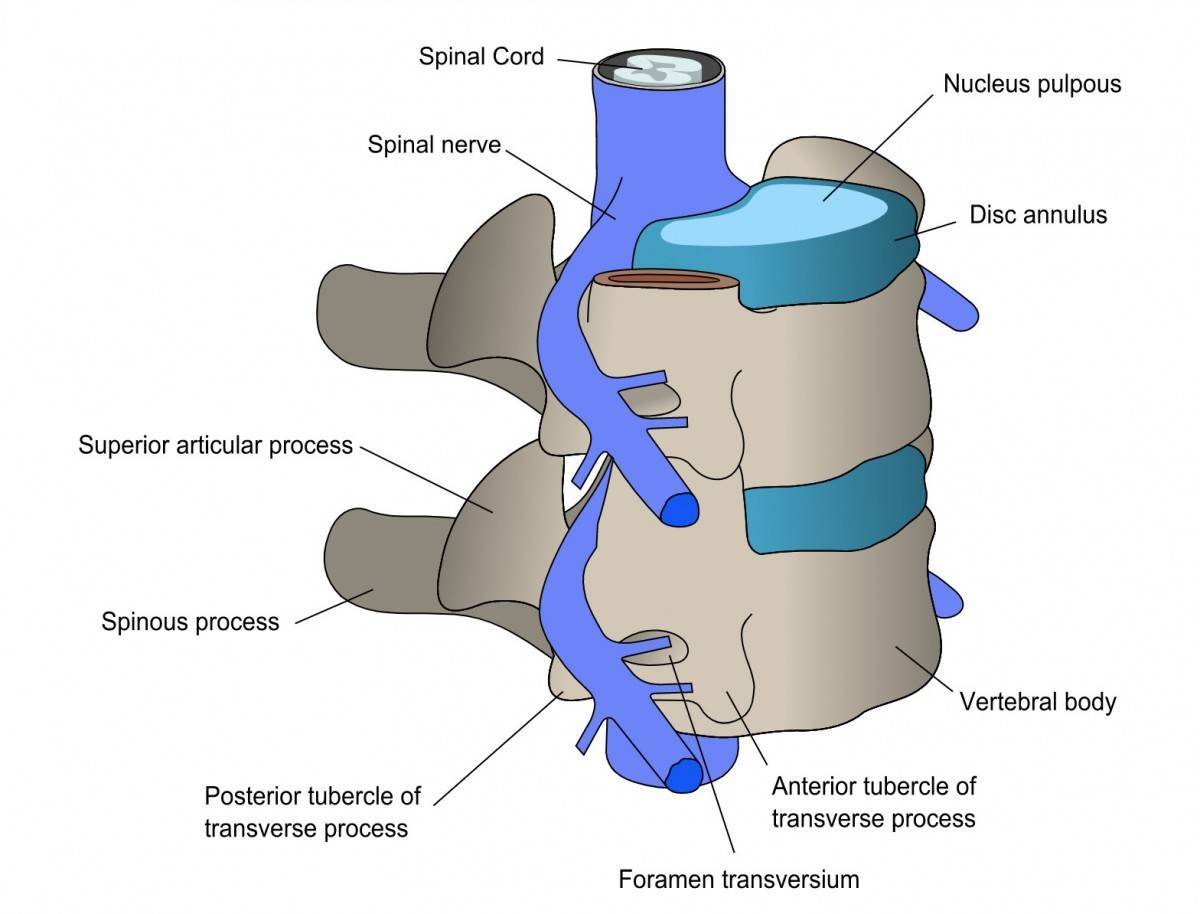
Slipped disc
The bones of the spine are cushioned by discs which absorb the shocks from daily activities like walking, lifting, and twisting. Injury or excessive pressure from lifting or pulling heavy objects can cause the outer ring to tear, allowing the inner portion of the disc to slip out. This is known as a slipped / prolapsed / herniated disc. It causes progressively severe pain and discomfort as the protruding soft core compresses spinal nerve(s).
Degenerative Disc Disease
This is an age-related wear-and-tear of intervertebral discs. As you age, the soft part of the discs (nucleus pulposus), which are made largely of water, may dry up and the discs thin out.
This allows the bones on either side of the disc to get closer together. As the bones get closer together, they experience more stress, and likewise the joints around the bones too. The bones and joints react by making bony growths (spurs), and over time these spurs begin to pinch the nerves. This pinching of the nerves can cause radicular pain most commonly in the neck (cervical spine) and lower back (lumbar spine) as these areas undergo the most motion/stress.
Sciatica/Lumbar Radiculopathy
It is pain along the path of the sciatic nerve, which radiates from your lumbar spine to your buttock and down the back of one leg. The pain may be mild or a sharp jolting one, with or without concomitant numbness and tingling. It is intense when you sit for a long time and may be aggravated on coughing or sneezing.
Spinal Stenosis:
It is caused by the narrowing of the canal through which the spinal cord passes between the vertebrae, thereby compressing the spinal cord and nerve roots branching out. This results in pain, weakness and sometimes numbness. Herniated discs and bone spurs are the most common causes for spinal stenosis. Other causes include:
- injuries, where dislocated bones and inflammation from damage occurring near the spine can narrow the canal space exerting pressure on spinal nerves
- cancer, where tumours within or around the spinal cord can narrow the canal and put pressure on spinal nerves
There are also non-musculoskeletal reasons for back pain e.g. presence of kidney stones, gallbladder problems.
Managing back pain
The following home remedies may help decrease the incidence of back pain:
- Adopting better posture – Taking a rest and changing positions from time to time while sitting for extended durations due to work is helpful. Do not bend forward, lean on one side, or lean back for a lengthy period. One way to sit straight perfectly is by drawing an imaginary vertical line straight up from your chair towards the roof and sitting along that line and holding your shoulders even.
- Using ergonomically designed chairs which support your back can be helpful
- Applying ice helps decrease inflammation and hence the pain
- Using a warm pad after 24 hours of applying ice helps ease the pain by improving blood circulation to the back
- Taking over-the-counter medicines such as painkillers or analgesic patches can alleviate more intolerable pain
- Doing yoga and getting a massage can help release and stretch the stiff muscles
- Doing stretching and certain exercises that help strengthen your back muscles
When to see a doctor?
Most of the time, managing back pain can be achieved with adopting better sitting posture and exercise. But consulting a doctor might be necessary in the following situations:
- Continuous pain that does not improve with time
- Numbness and pain that feels like electric currents
- Bowel and bladder function are lost
- Unintentional weight loss
- Fever
Recognising the symptoms and finding the cause of the back pain is the initial step in receiving helpful treatment. Back pain can present usually as acute pain (short-duration), chronic pain (long-duration) and neuropathic pain (nerve-related).
Doctors may advise imaging tests before prescribing medical treatments for back pain. Such treatments include physiotherapy, nerve blocks, steroid injections, laser therapy, acupuncture, and medications like muscle relaxants, antidepressants, etc. If all of the above measures fail, then surgery may be recommended.
Watch the video below, to listen to an Orthopaedic Surgeon talk more about managing your aches and pains: