What is COPD?
Chronic Obstructive Pulmonary Disease (COPD) is the progressive decline of lung function due to emphysema and/or chronic bronchitis. These conditions cause damage and inflammation to the lungs, manifesting as breathing difficulty and chronic cough with mucus. It is the third major cause of death worldwide. COPD affects people of both genders, though it is most commonly found in men. COPD is mainly caused by smoking, or chronic exposure to secondhand smoke and pollutants. It may be hereditary though rarely so, as in the case of alpha-1 antitrypsin deficiency (AATD), where the body does not produce sufficient alpha-1 antitrypsin protein to protect against the enzyme neutrophil elastase from attacking lung tissue.
How Does COPD Affect the Lungs?
To understand how COPD affects the lungs, we need to understand how the lungs normally function.
When we inhale, air enters from our nose/mouth and into the trachea (windpipe). The trachea branches into two bronchial tubes, one leading into the left lung, the other leading into the right lung. The two bronchial tubes branch out further into thousands of smaller air passages called bronchioles, which end in tiny air sacs called alveoli. When we breathe in, these alveoli expand; when we breathe out, they deflate. With each breath, oxygen moves through the capillaries in the alveolar walls into the blood. Carbon dioxide moves from the blood into the alveoli so we can exhale it back out.
In emphysema, the alveolar walls are damaged, and the alveoli lose their elasticity. Air gets trapped in the alveoli, making it hard to exhale. Wheezing (a high-pitched whistling sound) is caused by turbulent airflow on exhalation. In chronic bronchitis, the lining of the airways becomes inflamed, prompting thick mucus to form. This inflammation and excess mucus hinder normal breathing, often causing chronic cough. It can also lead to recurrent infections.
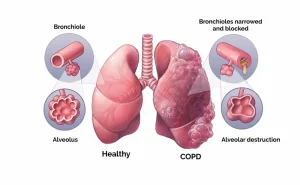
Diagram 1. How COPD causes damage to the lungs and cause breathing difficulties
How is COPD Diagnosed?
The doctor will first examine you and inquire about any family history of the condition for diagnosing COPD. The doctor will also ask you about your lifestyle, especially exposure to cigarette smoke.
In addition, the below tests will also be conducted to diagnose the condition:
Lung function test
Spirometry is a test that measures your lungs’ capacity to take in and blow out air. In this non-invasive test, you will be asked to blow into a tube connected to a machine. This test will help in ascertaining disease progression. Your forced expiratory volume (FEV1), a measurement of how much air you can force out of your lungs in one second, is compared to that of a person your age, height, and race, with normal, healthy lungs.
COPD is typically categorized into 4 stages according to the GOLD (Global Initiative for Chronic Obstructive Lung Disease) staging system:
- Stage 1: Very mild COPD with a FEV1 about ≥80% of normal
- Stage 2: Moderate COPD with a FEV1 between 50% and 80% of normal
- Stage 3: Severe emphysema with FEV1 between 30% and 50% of normal
- Stage 4: Very severe COPD with a lower FEV1 than Stage 3, or those with Stage 3 FEV1 and low blood-oxygen level
Arterial Blood Gas test
This involves taking a blood sample from an artery to measure your blood oxygen, carbon dioxide, and other important levels.
Chest x-ray
COPD can be caused by emphysema in which the alveoli in the lungs are destroyed. Chest x-ray allows visualization of damaged alveoli.
CT scan
A CT scan normally follows a chest x-ray. It provides a clearer picture of the lungs, and can also aid in detection of lung cancer.
Lab test
Lab tests are done to determine whether you have alpha-1 antitrypsin deficiency (AATD), which can be a main cause of COPD. This is done if you have a family history of COPD or develop COPD at a young age.
How is COPD Treated?
Lifestyle changes
The main lifestyle change to be made for treating COPD is quitting smoking or limiting tobacco exposure. This prevents COPD from getting worse. If self-control is not working, you can seek the help of your doctor, who will provide nicotine replacement products or medications that help you quit smoking. Being part of a support group also helps you to quit smoking.
In addition, you should lead adopt a healthy lifestyle with balanced nutrition, plenty of fluid intake and regular exercise. You should also go for doctor check-ups at regular intervals. Also practicing relaxation technique and energy conservation technique helps you to manage when you are short of breath.
Medication
Different types of medication are available that help to ease the symptoms of COPD. This includes
- Bronchodilators: These are available as inhalers and help to relax the muscles in your airway, widening the airways to make breathing easy and provide relief from cough. Depending on the severity of your condition, the doctor will prescribe a short-term or long-term bronchodilator. Few of the short-term bronchodilators are albuterol and levalbuterol. Long-term bronchodilators include formoterol and Indacaterol.
- Inhaled steroid: Inhaled corticosteroid medications can reduce inflammation in the airways and lower mucus production.
- Combination inhaler: This includes a combination of bronchodilators and inhaled steroid.
- Oral steroid: For those who get severe symptoms of COPD at certain intervals, short-term oral steroids for around five days may be prescribed. Long term use of steroids can have severe side effects. Thus, it is recommended to stop the medication after this short period.
- Antibiotics: Antibiotics may be prescribed for infections like pneumonia and influenza which can worsen the COPD.
- Vaccines: Vaccines e.g. yearly influenza shot may be useful to prevent other respiratory infections.
Lung therapy
- Oxygen therapy: Through oxygen therapy, regular supply of the oxygen to the lungs is ensured. Patients will be advised to carry portable units of oxygen while running errands. Some people will use oxygen when they are sleeping or engaging in some activities.
- Rehabilitation program: These programs combine diet, exercise, counselling and education to improve the quality of life. Different experts will examine you and then tailor a rehabilitation program that suits your lifestyle and health status.
Surgery
For those who do not get the desired result through medication, surgery may be prescribed. This includes:
- Volume reduction surgery: In this surgery, damaged tissues will be removed from the lungs. This provides extra space where healthy lung tissues can expand, and the diaphragm can work more efficiently.
- Transplantation: In case of lung transplantation, a healthy lung will be transplanted to the person’s body. This is a high-risk surgery which can sometimes result in organ rejection.
Conclusion
COPD requires lifelong management. Although there is no cure for COPD, you can slow its progression and ease symptoms with appropriate lifestyle changes, medications and regular follow up at the doctor’s. Having a support group of family and friends will also help you to cope with the condition and make the most out of life.
